These post-test questions are designated for attendees who have already watched all the lectures and wish to obtain CME credits through Johns Hopkins CME office.
- Patients with heart failure may have artifacts that mimic pulmonary emboli because:
- Pulmonary interstitial congestion obscures the pulmonary artery visualization
- Poor breathholding results in motion artifacts
- Mixing artifacts due to poor cardiac output can simulate filling defects
- Low level enhancement of the pulmonary arteries results in significant image noise
- Atrial septal aneurysms are:
- Prone to development of thrombus and are usually treated if >20 mm
- Frequently seen by CT and uncommonly seen by echocardiography
- Usually secondary to infection
- Incidentally encountered abnormalities that usually do not require follow-up
- Perigraft fluid in the post-operative state:
- Should be followed if >2 cm in thickness
- Is a normal finding if shrinking over time
- Tends to grow slowly
- When present indicates infection
- Surgical material from graft repair of the aorta:
- Is hypoattenuating on CT
- Is high signal on MRI
- Is hyperattenuating on CT
- Usually enhances
- What is the most likely diagnosis?
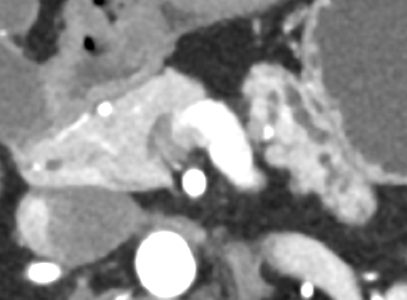
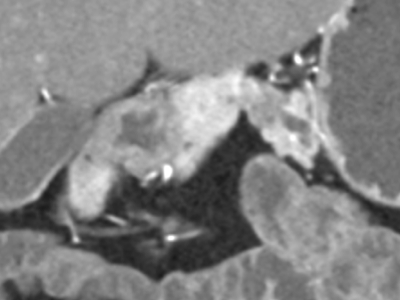
- Pancreatic ductal adenocarcinoma
- Chronic pancreatitis
- Autoimmune pancreatitis
- Normal
- Which of these statements about autoimmune pancreatitis is true?
- Normal serum IgG4 excludes diagnosis
- Diffuse hyperdense halo is typical
- Diffuse parenchymal calcifications are present
- Most patients respond to steroids
- What is the most likely diagnosis?
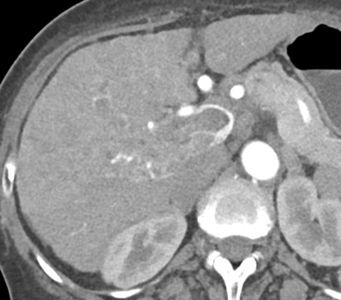
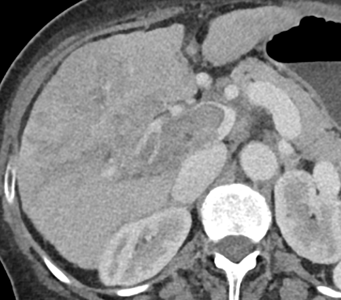
- Cholangiocarcinoma
- Hepatocellular carcinoma
- Metastatic disease
- Hypercoagulable state
- Calcifications are usually seen in which of these masses?
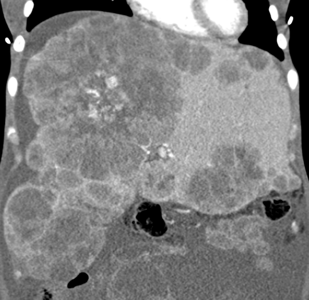
- Hemangioma
- Focal nodular hyperplasia
- Abscess
- Metastases from mucinous colon cancer
- What is the most common form of necrotizing pancreatitis:
- Pancreatic parenchymal and associated peripancreatic necrosis
- Peripancreatic necrosis alone
- Pancreatic parenchymal necrosis alone
- Pancreatitis presenting with walled-off necrosis
- 60-year-old man with acute pancreatitis.
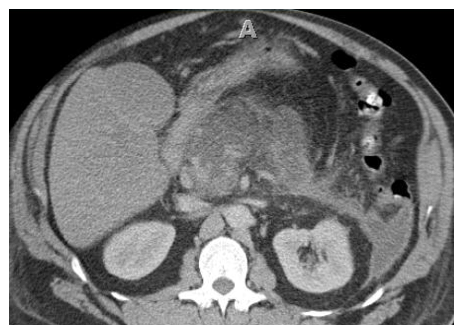
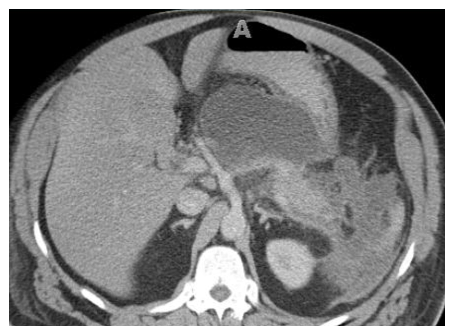
A B Image A was acquired at the time of presentation and image B at 7 weeks later for persistent abdominal pain. The correct term for the complication in image B:
- Necrotizing pancreatitis
- Walled-off necrosis
- Pseudocyst
- Acute peripancreatic fluid collection
- In the National Lung Screening Trial (NLST), what was the reduction in lung cancer mortality in the computed tomography (CT) group compared to the control group?
- 10%
- 20%
- 30%
- Which of the following modality is used for lung cancer screening?
- High-resolution chest CT
- Conventional-dose chest CT with contrast
- Low-dose chest CT without contrast
- A growing 1 cm solid nodule was detected on a recent screening chest CT. Which of the following is the most appropriate next test for the patient?
- FDG-PET/CT
- Follow-up CT in 3 months
- MRI chest without and with IV contrast
- The most common extrapancreatic involvement of AIP involves which of the following organs:
- Kidneys
- Biliary tree
- Small bowel
- Thyroid
- Type 1 AIP is usually seen in younger patients compared to type 2 AIP.
- True
- False
- The ADC values of AIP tend to be lower than that of PDAC?
- True
- False
- CT shows peribronchovascular reticular opacities with traction bronchiectasis and subpleural sparing. Mosaic attenuation and honeycombing are absent. What is the most likely pattern?
- Chronic hypersensitivity pneumonitis
- Lymphocytic interstitial pneumonia
- Nonspecific interstitial pneumonia
- Usual interstitial pneumonia
- The "straight-edge" sign, "exuberant honeycombing" sign, and "anterior upper lobe" sign are most commonly found in which of the following diseases?
- Asbestosis
- Connective tissue disease-associated interstitial lung disease
- Cryptogenic organizing pneumonia
- Sarcoidosis
- CT shows an avidly-enhancing endobronchial mass. What is the most likely diagnosis?
- Adenoid cystic carcinoma
- Carcinoid
- Hamartoma
- Mucoepidermoid carcinoma
- Which of the following is most likely associated with bronchiectasis?
- Allergic bronchopulmonary aspergillosis
- Bronchial asthma
- Tracheobronchial amyloidosis
- Relapsing polychondritis
- Most renal masses under 1 cm in size are?
- Malignant
- Need to be resected unless a classic cyst
- Angiomyolipomas
- Can be followed conservatively even if not definitely a simple cyst
- CT can be used to distinguish clear cell renal cell carcinoma from papillary renal cell carcinoma is over 90% of cases based on
- Lesion size
- Enhancement of the mass on arterial phase imaging (HU)
- Enhancement on excretory phase imaging (HU)
- Presence of calcification
- Positive oral contrast is no longer needed in the ER setting.
- True
- False
- Faster injection rates (i.e. 5cc/sec) are the main cause of contrast extravasation.
- True
- False
- Which of the following tumors is most common in the duodenum?
- Adenocarcinoma
- Lymphoma
- Carcinoid tumor
- GIST
- B-cell lymphoma is the most common type of small bowel lymphoma in the US.
- True
- False
