Gastric Pathology: The Current Role of CT in Imaging the Stomach
Karen M. Horton , MD and Elliot K. Fishman, MD
ABSTRACT
Recent advancement in CT scanners and computer technology has renewed interest in utilizing CT for the evaluation of gastric pathology. Multidetector Row scanners allow thinner collimation, which improves the visualization of subtle tumors and also improves the quality of the 3D data sets. When water is used as oral contrast, subtle pathology is easier to visualize, especially when a good IV contrast bolus is administered. Adenocarcinoma is the most common gastric malignancy and typically appears as focal or segmental wall thickening or as a discrete mass. Gastric lymphoma can have a similar CT appearance to adenocarcinoma. Both gastric adenocarcinoma and lymphoma may has associated adenopathy. Gastrointestinal stromal cell tumors tend to appear as well defined masses which arise from the gastric wall and may be exophytic when large. These tumors are usually not associated with significant adenopathy. In addition to gastric malignancies, CT can also detect inflammatory conditions of the stomach, including gastritis and peptic ulcer disease. CT angiography is helpful to better define the gastric vasculature which may be affected by a variety of conditions.
ONE SENTENCE
This article discusses the use of spiral CT and MDCT as well as 3D imaging for the evaluation of patients with suspected gastric pathology including gastric malignancies and inflammatory conditions.
INTRODUCTION
Recent advancements in CT technology including the introduction of multidetector row CT (MDCT) and the development of real-time 3D imaging systems have renewed interest in utilizing CT for evaluation of the gastrointestinal tract. The same technology which is applied to CT colonography, the generation of 3D and endoluminal views of the colon, can be used to obtain a detailed CT examination of the stomach. For dedicated gastric imaging, water is used as oral contrast. The water is well tolerated and results in good gastric distention as well as excellent visualization of the enhancing gastric wall. Volume rendering of CT data coupled with interactive 3-D and stereoscopic display can then be used to better visualize gastric pathology.
This article discusses the use of spiral CT and MDCT as well as 3D imaging for the evaluation of patients with suspected gastric pathology including gastric malignancies and inflammatory conditions. A detailed discussion of CT scanning protocols and 3D imaging techniques are provided.
TECHNIQUE
Oral Contrast
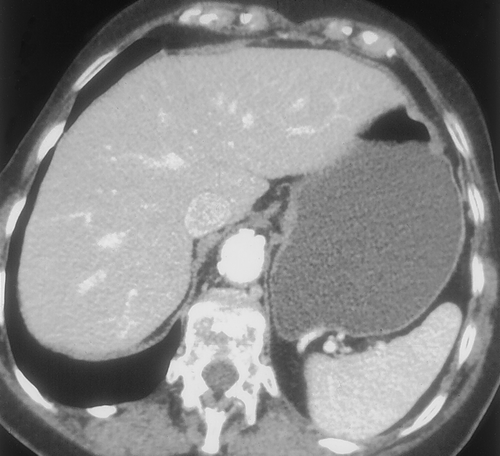
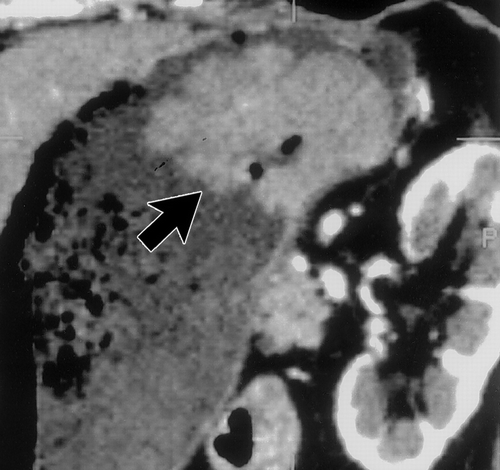
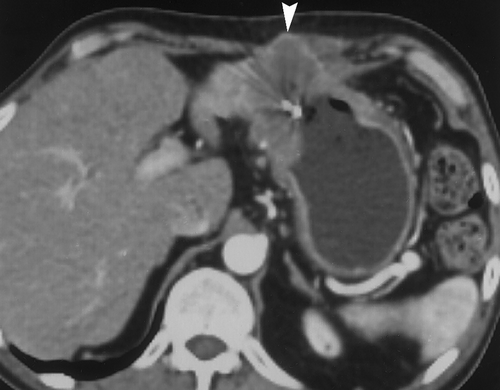
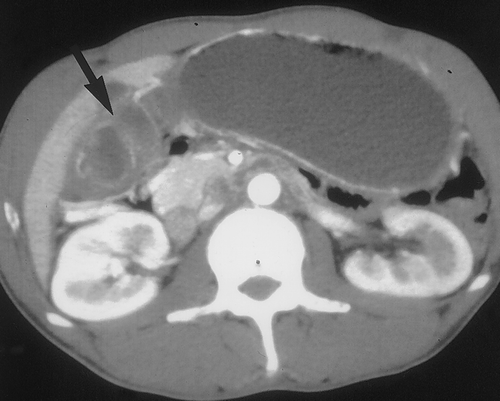
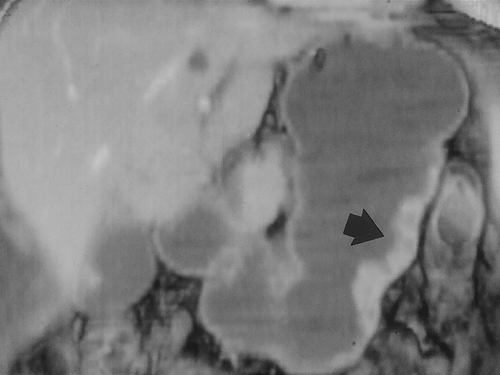
For dedicated imaging of the stomach, adequate distension is essential. If the entire stomach is not well distended, pathology may be overlooked, or conversely, the collapsed gastric wall may mimic disease. Traditionally high attenuation contrast agents have been administered to opacify and distend the stomach and gastrointestinal tract. These agents can be categorized as positive contrast, as they have an attenuation greater than water on CT scans. Although these agents are safe, well tolerated and result is good gastric distension, they may not be optimal when evaluating the GI tract and stomach in particular. Occasionally positive oral contrast may not mix uniformly with gastric contents and pseudotumors can be created, both on the axial images and endoluminal views1. Since the wall of the GI tract can enhance up to 120 HU after the administration of intravenous contrast, the high density intraluminal contrast may mask subtle pathology2 (Figure 1). Also, the use of positive agents can complicate 3D imaging and CT angiography in particular, by necessitating extensive editing since the positive contrast may obscure opacifed vessels.
Recently there has been interest in utilizing alternative oral contrast agents for gastrointestinal tract imaging with CT. There is an advantage to using low attenuation agents with attenuation values similar to water. These agents allow better evaluation of the enhancing gastric wall and may allow better detection of subtle pathology3, 4 (Figure 1). In addition, low density agents would not interfere with 3D imaging and CT angiography3. Oil based oral contrast agents have been tested and do allow adequate depiction of the stomach wall, but are not very palatable and result in significant steatorrhea, although newer preparations may be better5. Whole milk has been proposed as a possible CT oral contrast and is used by some groups routinely when performing CT angiography6. Milk is emptied relatively slowly from the stomach and has a slower small bowel transit time than water. However, many adults are lactose intolerant and therefore may experience cramping and diarrhea.
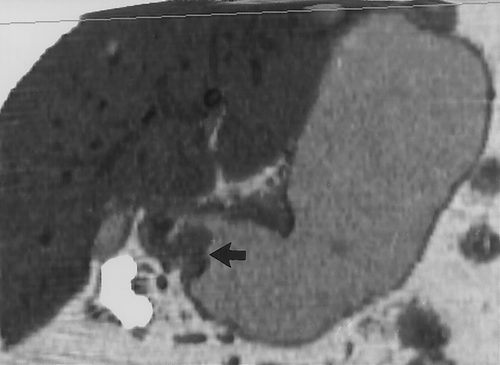
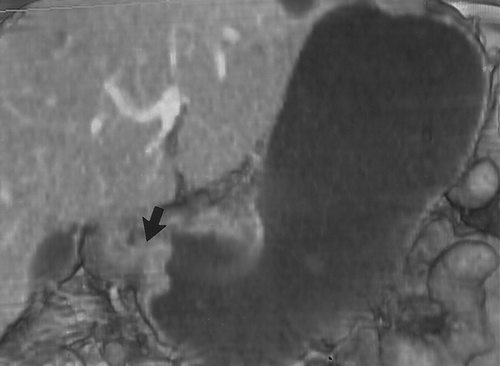
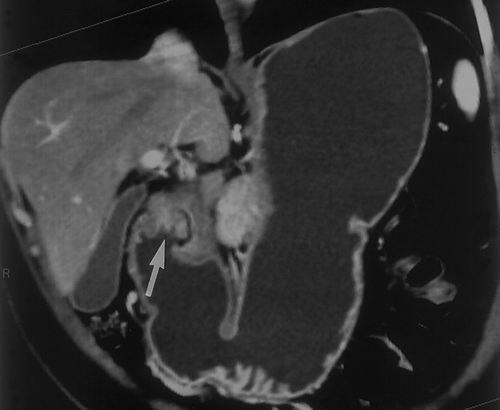
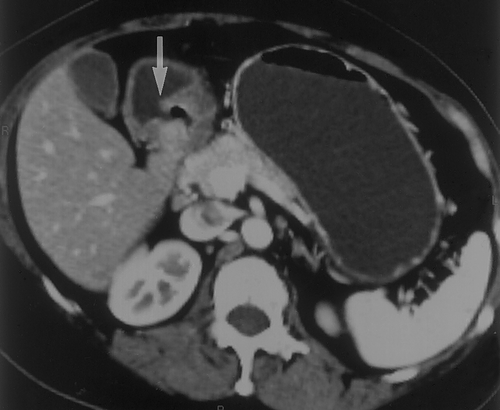
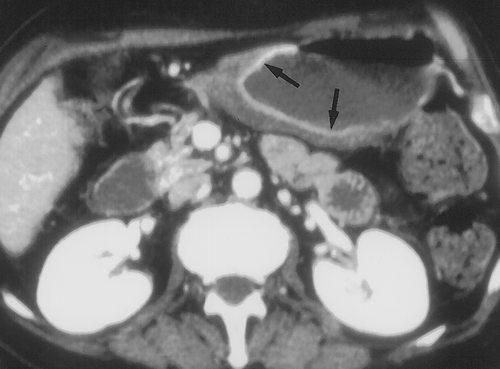
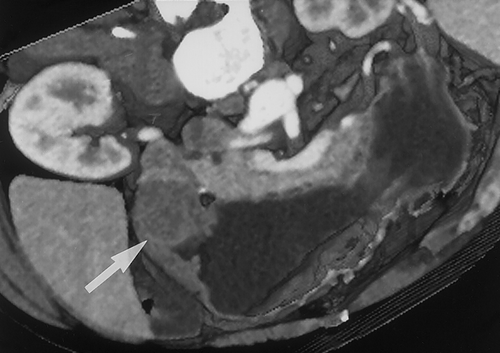
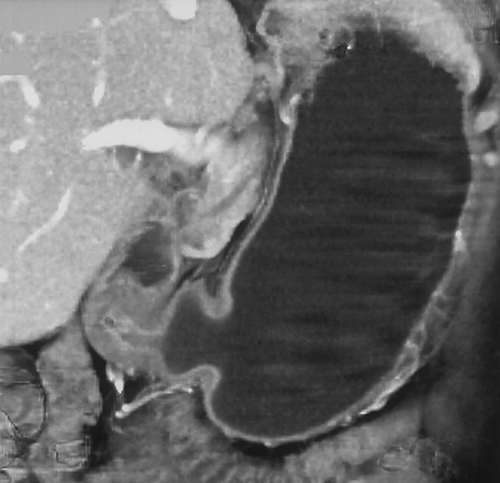
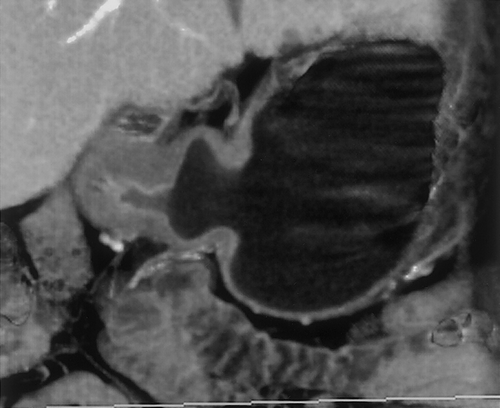
We prefer to use water for oral contrast in patients with suspected gastric pathology. Water is inexpensive (usually free) and well tolerated4. It distends the stomach well, allows good visualization of the enhancing wall and does not interfere with the manipulation of the 3D data sets (Figures 2 & 3) . When performing CT to specifically evaluate the stomach. 750cc of water is given to the patient approximately 15 minutes before the study. An additional 250cc is given immediately prior to the study. If necessary, air crystals can also be given. This is only rarely necessary, but can be helpful to better distend the gastric cardia and gastroesophageal junction. For optimal distension of all parts of the stomach, some authors have suggested combining prone and supine imaging, although we rarely find this necessary in our practice7. In addition, in certain cases, decubitus imaging may help distend the gastric antrum and pyloric region.
One disadvantage of using water is that it results in suboptimal distention of the distal small bowel. Some authors have advocated giving positive contrast initially, followed by water8. The positive contrast will fill the distal small bowel loops while the water will distend the stomach and proximal small bowel8.
IV Contrast
In addition to oral contrast for good gastric distention, intravenous contrast is essential for complete evaluation of neoplastic and inflammatory diseases of the stomach. We routinely administer 120 cc of non-ionic contrast (Omnipaque 350, Nycomed-Amersham, Princeton, NJ) at a rate of 3 cc per second.
Scan Protocol
Gastric imaging has been improved by the introduction of multiple detector row scanners. We currently use a Siemens Somatom Volume Zoom (Siemens Medical Systems, Iselin, NJ) which can be 8 times faster than traditional 1 second single detector row spiral scanners. Depending on the collimator setting, the Volume Zoom can acquire up to 4 slices per 0.5 sec rotation. This almost eliminates motion artifacts. Also these scanners allow thinner slices than single detector spiral scanners. 0.5mm slices are easily obtainable. The thinner collimation definitely improves the quality of the 3D data set, in terms of gastric imaging as well as CT angiography. It is important to realize that the radiation dose to the patient increases when thin collimation is used. It is therefore crucial to monitor exactly what dose an individual patient receives. Also newer MDCT scanners incorporate features to help minimize the patient radiation exposure buy modulating the dose according to the individual's body habitus.
When imaging a patient with known gastric pathology, we utilize the 4 x 1.0 mm collimator setting. 1.25 mm slices are then generated and reconstructed at 1 mm intervals. The overlap improves the quality of the 3D imaging. Using this setting, the abdomen (diaphragm to iliac crest ) can be scanned in 20 seconds. MDCT offers considerable flexibility and therefore although the 1.25-mm slices are utilized for the 3D images, the data can also be reconstructed with 3-5mm slices for routine review on film or a workstation. In patients undergoing CT for follow-up after gastric surgery, 3mm slices are usually adequate..
Depending of the indication, dual phase imaging may be performed. Arterial phase images are acquired 25 seconds after the start of the injection, venous phase images are acquired 50 seconds after the start of the injection, using identical technique (1.25mm slices reconstructed at 1mm interval). This allows optimal visualization of both the gastric arteries and veins.
3D Imaging
3D imaging of the gastrointestinal tract, the colon in particular, has gained much attention since it was first proposed in 1993. At that time, 3D imaging was limited by computer speed and performance. Early reports of 3D CT imaging of the stomach (CT gastroscopy) were limited to surface rendering techniques, i.e. shaded surface. However, with improvements in computer technology and speed, most manufacturers now also offer volume rendering. Shaded surface only displays information from the surface of the volume, while VR can display all attenuation values throughout the data set1, 9. Therefore, VR is superior to shaded surface for imaging the stomach and gastric vessels. We currently use the Siemens 3D Virtuoso Imaging package. This software includes real-time volume rendering as well as flythrough capabilities.
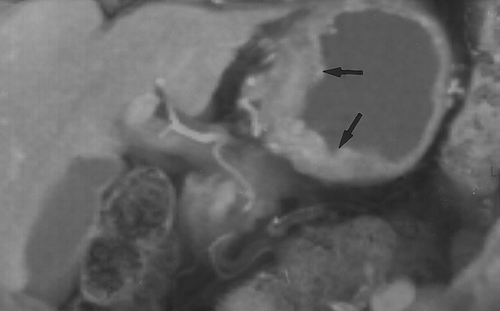
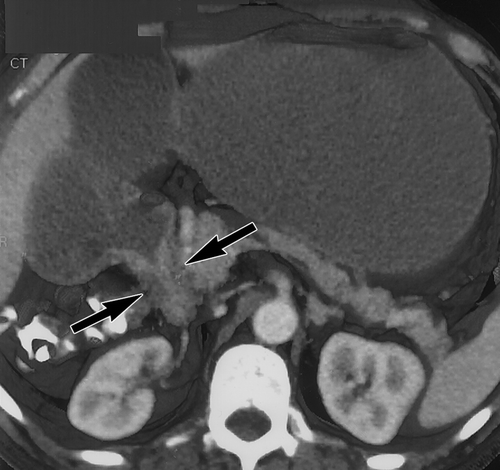
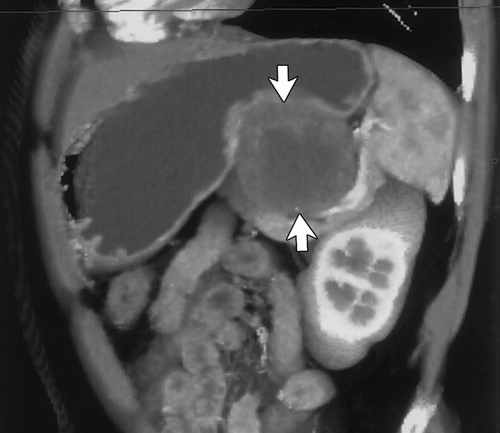
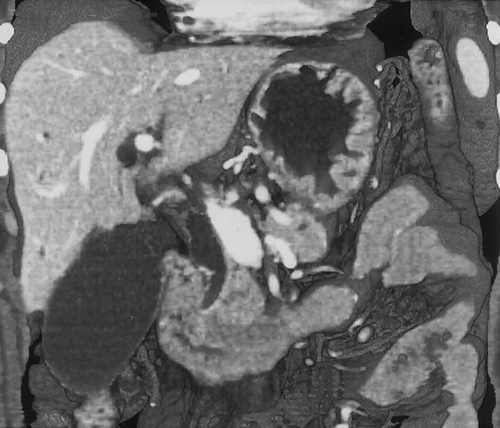
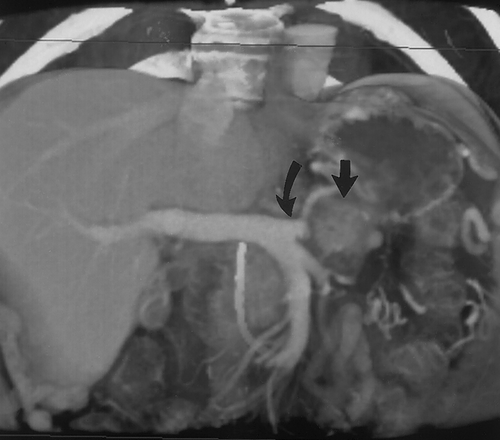
At our institution, after the data is acquired (1.25mm slices reconstructed at 1 mm intervals) it is transferred over an Ethernet to a Infinite Reality or Onyx workstation with Reality Engine graphics (Silicon Graphics, Mt. View, CA) or an O2 workstation for interactive volume rendering. Simple 2D multiplanar reconstructions of the CT data allow quick visualization of the stomach in the axial, sagittal and coronal planes. Most radiologists are familiar and comfortable with 2D MPR. It is quick and available on all workstations. An abnormality detected in one plane can immediately be visualized in the other two planes (Figure 4). The ability to visualize an abnormality in multiple planes, increases confidence and helps to better characterize the morphology of the lesion. It is often helpful to start with the MPR and then proceed with the 3D. The main advantage of 3D volume rendering over 2D MPR is the added perspective and enhanced depth perception. A torturous vessel or complex mass can be visualized in its entirety with 3D and its relationship to adjacent structures can be better appreciated.
The 3D volume set can be manipulated using different orientations or cut planes in order to best demonstrate the stomach and pathology. For gastric pathology it is often helpful to display the stomach in a coronal or coronal oblique plane if possible. The referring physicians especially appreciate this orientation, as the image is then similar to an upper GI series. This flexibility is a distinct advantage over traditional axial images. In addition to the use of cut-planes, the radiologist has the ability to change the opacity, brightness, window width and level. This allows the radiologist to accentuate certain structures. For example, When CT angiography is performed, the settings can be optimized to display the vessels, and the adjacent soft tissues will become transparent. In addition, the settings can be altered so that the appearance of the water filled stomach is similar to a traditional CT. Alternatively, the parameters can be altered to change the appearance of the gastric wall and intraluminal water. This may help accentuate certain pathology (Figure 5).
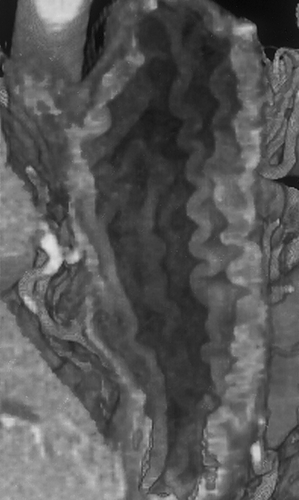
In addition, the CT data of the stomach can be also be manipulated to simulate images as seen by the endoscopist for "virtual gastroscopy". This display technique accentuates the stomach wall and folds (Figure 6). Early studies of this technique were limited, mostly due to computer limitations1. In a study by Springer et al of both cadavers and patients the endoluminal views using shaded surface display correlated well with endoscopy except for artificial smoothing of surface structures and density limitations created by the shaded surface technique1. The quality of virtual gastroscopy should be improved by the use of the thinner collimation possible with MDCT scanners and now that volume rendering can be performed easily and in real-time. Often it is not necessary to travel through the "stomach" as is done in virtual colonoscopy, but instead, the radiologist can simply use the clip planes and different orientation to completely visualize the entire stomach.
GASTRIC PATHOLOGY
Neoplasms
Adenocarcinoma
Adenocarcinoma is the most common gastric malignancy, representing over 95% of malignant tumors of the stomach10, 11. It is an aggressive tumor with a 5 year survival rate of less than 20 %9. Prognosis is correlated to the stage of the tumor at presentation. Therefore, accurate staging of gastric cancer is essential, as surgical resection is the treatment for localized disease. CT is currently the staging modality of choice since it can identify the primary tumor, assess for local spread, as well as detect nodal involvement and distant metastases.
Several studies have evaluated the benefit of using water as oral contrast for detection and staging gastric malignancies12-14. In a study by Hori at al using water as oral contrast, CT detected 95% of advanced carcinomas (with local invasion or metastatic disease), 93% of elevated early carcinomas (no local invasion or metastases), and 18% of early depressed carcinomas13. In a similar study by Baert, 22/24 (91%) of gastric carcinomas were detected. In a study by Rossi et al using water as oral contrast and glucagon for hypotonia, the accuracy for staging gastric cancer was 66-77%. The major limitation in that study was difficulty determining the level of tumor invasion in the gastric wall12.
When water is used as oral contrast, gastric tumors appear as segmental or diffuse wall thickening which may demonstrate different enhancement from the normal adjacent gastric wall (Figure 4, 5 & 7) . These tumors may be subtle, but are easier to detect if low density oral contrast is present (Figure 8 & 9).
In addition to the use of water as oral contrast for the detection and staging of gastric malignancies, there may be an advantage to performing dual phase dynamic contrast enhanced CT15. Hundt et all studied 40 patients with gastric malignancies using dual phase CT (arterial and venous phase) and water as oral contrast. 39/40 (97.5%) cancers were detected. The CT staging correlated with the pathologic staging in 79.4%15. The major limitation in staging was the difficulty in correctly detecting tumor invasion of nodes. In a study by Mani et al of 20 patients with gastric cancer , two phase CT was performed at 45 sec and 3 minutes after the injection of IV contrast16. Water was given as oral contrast. The earlier phase (45s) was highly accurate for determining the depth of tumor invasion through the wall16. The authors correctly determined the depth of tumor invasion in 17/20 patients16. The later phase (3 min) did not add any additional information. However, the addition of an arterial phase (25 seconds) was not performed in this set of patients. Arterial phase imaging would be beneficial for vascular imaging and often accentuates the differences in the appearance between the normal gastric wall layers and tumor. Arterial phase imaging also better display the gastric arterial anatomy which may be important if there is local extension of tumor. However, the optimal protocol (arterial, venous, delayed) for detection and staging of gastric malignancies is still under investigation.
Axial images have always been useful when staging gastric malignancies. However, multiplanar reconstructions and 3D images provide additional valuable information and improve detection and staging of both early and advanced tumors 9, 17, 18 (Figure 8). In a study by Lee et al of 31 patients with early gastric cancer, the tumor detection rate was higher using 3D imaging compared with using axial images alone (93.5% vs. 64.5 %)17. In another study by Lee et al of 60 patients with advanced gastric malignancies, the combination of 3D imaging with axial images improved the accuracy of tumor staging compared with axial images alone18. In those studies, shaded surface (SS) techniques were utilized for the 3D images. Results may even been better if volume rendering (VR) were used, since VR has been shown to be superior to SS for mucosal detail19.
In addition to 3D images for the stomach, endoluminal imaging is possible1, 9, 20. This provides a view similar to the endoscopist (Figure 6). Using this technique, it is possible to simultaneously visualize the primary tumor as well as extraluminal extension. One limitation to this technique is the difficulty detecting flat lesions, involving the mucosa only7, 9.
Lymphoma
The stomach is the most frequent site of gastrointestinal tract involvement by Non-Hodgkins lymphoma21. On CT, gastric lymphoma typically appears as segmental or diffuse wall thickening (Figure 10 & 11) . In a study of 12 patients with gastric lymphoma by Buy et al in 1982, the average gastric wall thickness was 4.0 cm, and in contrast to gastric adenocarcinomas, lymphoma typically involves more than one region of the stomach22. Using water as an oral contrast it may now be possible to detect cases in which the gastric wall is only minimal thickened. Since lymphoma is considered to be a "soft" tumors, it is less likely to result in gastric outlet obstruction than gastric adenocarcinoma.
Perigastric adenopathy is common in patients with gastric lymphoma as well as in patients with gastric adenocarcinoma. However, adenopathy which extends below the renal hila favors gastric lymphoma over adenocarcinoma22. In addition to detecting gastric involvement by lymphoma, CT is useful in detecting complications such as perforation, extragastric extension or fistulization21.
Mucosa-associated lymphoid tissue (MALT) lymphoma is a low grade lymphoma which is being recognized with increased frequency. It is though to be associated with Helicobacter pylori23. This tumors differ from the typically high grade Non-Hodgkin gastric lymphoma. In a series of 40 patients with gastric MALT lymphoma by Kessar et al, the most frequent finding was gastric wall thickening24.The wall thickening is usually minimal and my not be detected on CT, especially is the stomach is not maximally distended. Associated adenopathy or extragastric distention is not common 23-25.
Since the most frequent CT finding in both gastric lymphoma and gastric MALT lymphoma is wall thickening, careful attention to the CT technique is necessary. The stomach should be maximally distended. Again, water may allow better evaluation of the enhancing gastric wall. In some cases the addition of air my also be helpful. There are no studies addressing the utility of using water as oral contrast or using 3D imaging in the detection or staging of gastric lymphoma. However, in our experience we find this technique helpful, especially in subtle or complicated cases. In addition, the referring physicians and surgeons find the 3D images useful for treatment planning. In many cases the 3D CT images will obviate the need for other radiological studies such as the upper GI series.
Gastrointestinal Stromal Tumors (GIST)
Gastrointestinal stromal tumors are uncommon neoplasms which arise from mesenchymal cells in the wall of the gastrointestinal tract. These tumors demonstrate variability in differentiation and are categorized based on immunohistiochemical and ultrastructural studies26. Stromal tumors can be classified histiologically as myogenic (arising from smooth muscle), neurogenic (arising from neural elements) or less differentiated tumors, referred to as GIST. Stromal tumors with smooth muscle differentiation were formerly called leiomyoma/leiomyosarcoma. They account for only 1% of gastric tumors27, and usually occur in adults. CT is useful in the detection of these neoplasms28.
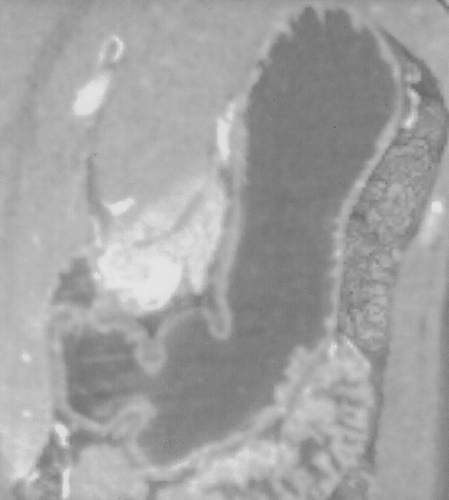
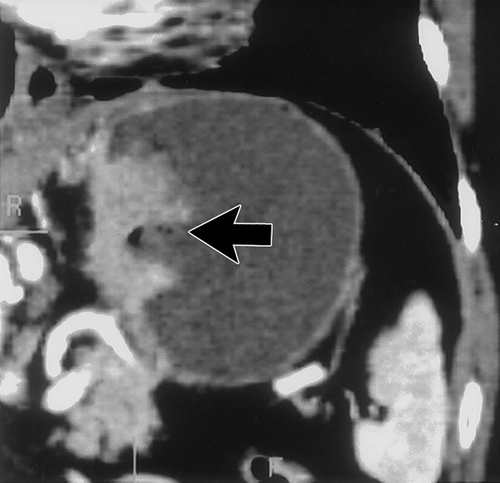
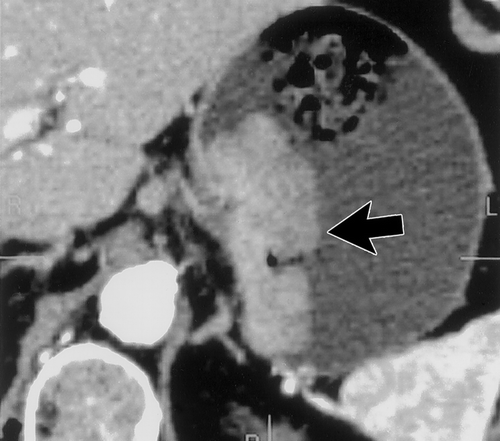
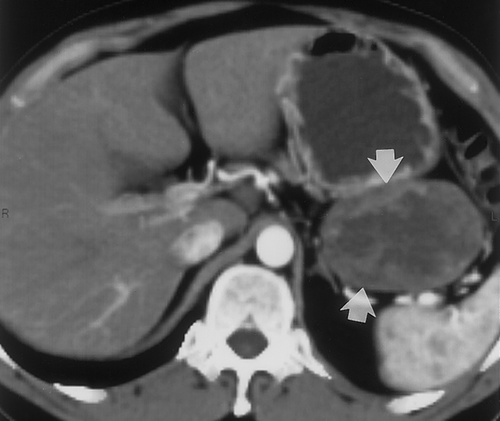
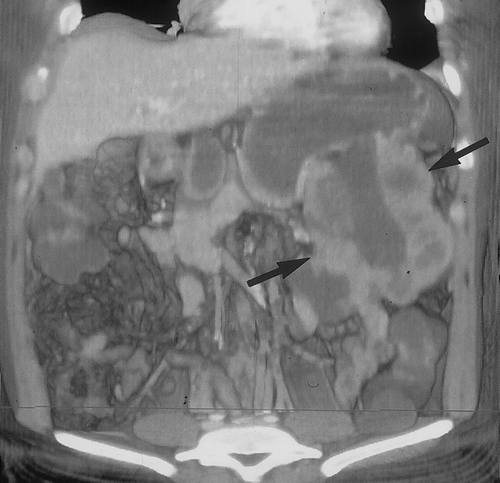
On CT, these tumors vary in appearance and size. 90% of gastric leiomyosarcomas occur in the fungus or body of the stomach29. Small tumors will appear as intramural masses (Figure 12) . As the tumors grow, they stretch the overlying mucosa and can ulcerate28. When large (>5cm), the tumors often appear grow exophytic and may contain areas of central necrosis or calcification27, 28 (Figures 13 & 14). When tumors are large and exophytic, it may be difficult to determine their site of origin, and in these cases 3D imaging can be helpful to better characterize the mass and to determine its origin. Adenopathy is uncommon, unlike patients with gastric adenocarcinoma or lymphoma.
Malignant stromal tumors can invade adjacent organs and can metastasize hematogenously, usually to the lung or liver. Metastatic lesions may also appear low in density due to necrosis.
CT cannot usually differentiate between malignant and benign gastric stromal tumor unless obvious local invasion or metastatic disease is detected. However, small tumors (<4-5cm) are usually benign. Resection and histiological analysis of mitotic activity and markers is necessary.
Inflammatory conditions
Infalmmatory Conditions
Gastritis
CT is not the imaging modality of choice in patients with suspected peptic ulcer disease. However, CT is often performed in patients presenting with nonspecific complaints such as abdominal pain and nausea. Therefore, CT may be the first study performed and may suggest the diagnosis.
The most common CT finding in patients with gastritis, is thickening of the gastric folds and wall (Figure 15) . In severe cases the gastric wall will demonstrate low density compatible with submucosal edema and inflammation10. At the same time the mucosa may enhance due to hyperemia. This may result in a layered appearance to the wall which is most pronounced on arterial phase imaging. This layering or halo will help distinguish gastritis from other conditions which thicken the gastric wall such as neoplasms. Neoplasms will not respect the layers of the gastrointestinal tract wall and will therefore not result in this striated or halo appearance. Gastritis does not have to involve the stomach diffusely and thus can appear as focal or segmental thickening. Helicobacter pylori gastritis in particular can simulate a gastric neoplasm, as it often results in circumferential antral wall thickening or focal thickening along the greater curvature30 (Figure 16 ). Other condition such as adult hypertrophic pyloric stenosis can appear as segment wall thickening (Figure 17). Since the CT appearance of gastritis and tumors can overlap, endoscopy is often necessary for definitive diagnosis. The role of 3D CT is in the evaluation of inflammatory conditions of the stomach has not been well studied.
Peptic Ulcer Disease
In patients with peptic ulcer disease, gastric ulcers are common in addition to gastritis. Most gastric ulcers are not visible on CT since they effect the superficial layers of the gastric wall31. However, deep ulcers or ulcers which have penetrated or perforated through the gastric wall can be detected. Patients with ulcer penetration may demonstrate inflammatory changes in adjacent soft tissue in addition to gastric wall thickening31. Perforation appears as inflammatory changes as well as extraluminal air bubbles or pneumoperitoneum.
Emphysematous Gastritis
Emphysematous gastritis is an uncommon entity usually caused by invasion of the gastric wall by a gas-producing organism, typically e.coli10, 32. This is a life-threatening condition with a mortality rate of up to 80%. On CT, the stomach is thickened and there is air within the layers of the wall. Air within the wall of the stomach can rarely occur after caustic ingestion or gastric infarction. In addition, there is a benign condition called gastric emphysema which may also result in air within the gastric wall. In fact, gastric emphysema is seen more commonly in clinical practice than emphysematous gastritis. The CT appearance of these two entities can be identical. However, patients with benign gastric emphysema are asymptomatic and the condition tends to resolve spontaneously10.
Gastric Varices
Gastric varices can occur in association with esophageal varices in patients with cirrhosis and portal hypertension. In these patients there is increased resistance to portal flow into the liver. Therefore, blood must find and alternative pathway to the heart, which includes the perigastric and periesophageal vessels. Isolated gastric varices, without esophageal varices can also occur in patients with splenic vein thrombosis or occlusion. This is typically seen in patients with pancreatitis and splenic vein thrombosis or in patients with pancreatic cancer with invasion and occlusion of the splenic vein (Figure 18) .
CT is valuable for detection of gastric varices and for identification of the underlying cause33. Gastric varices appear as enhancing tubular vessels , located primarily along the body and fundus of the stomach (Figure 18). Because they are veins, they will opacify during the portal venous phase of enhancement, and typically will not enhance on early, arterial phase studies. Collateral vessels are also commonly seen along the gastrohepatic ligament and along the course of the left gastric vein10. Gastric varices can be mistaken for gastric wall thickening, gastric cancer or perigastric adenopathy, if IV contrast is not administered. In patients with cirrhosis and portal hypertension, esophageal varices will also be present.
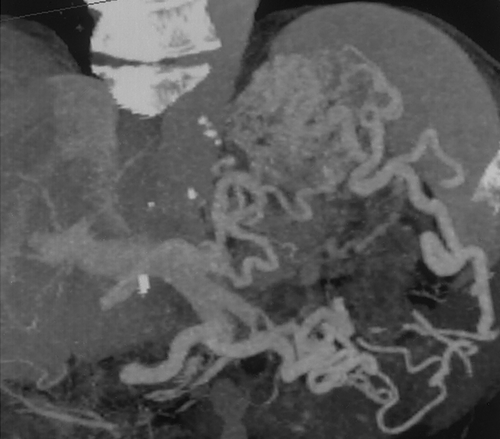
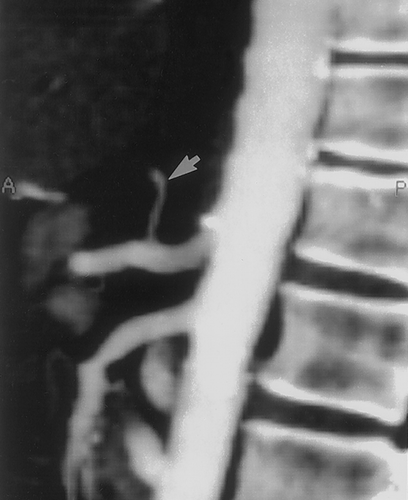
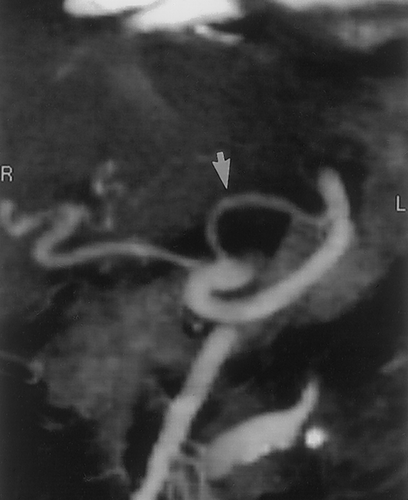
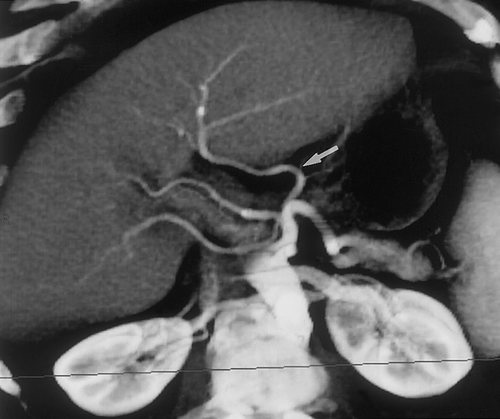
CT angiography is useful for detection of gastric varices. In a study by Matsumoto et al of 30 patients with gastric varices, demonstrated close agreement between the findings on 3D CT and conventional angiography34. In fact in four patients posterior gastric veins or short gastric veins were identified on 3D CT and not at conventional angiography. In this study, 3D CT studies were also used to evaluated patients after balloon occlusion of the varices34. The unlimited imaging planes possible with 3D CT imaging is definitely an advantage in trying to identify the small perigastric vessels. In addition to detection of gastric varices, CT angiography can routinely identify the arteries and veins which supply the stomach as well as anatomic varians34, 35 (Figures 19& 20).
CONCLUSIONS
Recent advancements in CT technology and 3D imaging software has renewed interest in utilizing CT for evaluation of gastric pathology. Detailed CT examinations of the stomach can routinely be obtained when water is used as oral contrast along with a good IV contrast bolus and the thin collimation obtainable with new multiple detector row CT scanners. 3D imaging of the stomach is helpful in the detection and evaluation of gastric malignancies and a variety of inflammatory condition which effect the stomach. CT angiography is especially useful for identifying the perigastric vasculature and gastric varices.
FIGURES
REFERENCES
1. Springer P, Dessl A, Giacomuzzi SM, et al. Virtual computed tomography gastroscopy: a new technique. Endoscopy 1997; 29:632-634. Medline
2. Horton KM, Eng J, Fishman EK. Normal enhancement of the small bowel: evaluation with spiral CT. J Comput Assist Tomogr 2000; 24:67-71. Medline
3. Horton KM, Fishman EK. Helical CT of the stomach: evaluation with water as an oral contrast agent. AJR 1998; 171:1373-1376. Medline
4. Winter TC, Ager JD, Nghiem HV, Hill RS. Upper gastrointestinal tract and abdomen: water as an orally administered contrast agent for helical CT. Radiology 1996; 201:365-370. Link
5. Ramsay DW, Markham DH, Morgan B, Rodgers PM, Liddicoat AJ. the use of dilute cologen as a fat density oral contrast medium in upper abdominal computed tomography, compared with the use of water and positive oral contrast media. Clin Radiol 2001; 56:670-673. Medline
6. Thompson SE, Raptopoulos V, Sheiman RL, McNicholas MM, Prassopoulos P. Abdominal helical CT: milk as a low-attenuation oral contrast agent. Radiology 1999; 211:870-875. Link
7. Ogata I, Komohara Y, Yamashita Y, Mitsuzaki K, Takahashi M, Ogawa M. CT evaluation of gastric lesions with three-dimensional display and interactive virtual endoscopy: comparison with conventional barium study and endoscopy. AJR 1999; 172:1263-1270. Medline
8. Matsuoka Y, Masumoto T, Koga H, Suzuki K, et al. Positive and negative oral contrast agents for combined abdominal and pelvic helical CT: first iodinated agent and second water. Radiat Med 2000; 18:213-216. Medline
9. Lee DH. Two-dimensional and three-dimensional imaging of gastric tumors using spiral CT. Abdom Imaging 2000; 25:1-6. Medline
10. Fishman EK, Urban BA, Hruban RH. CT of the Stomach: spectrum of disease. RadioGraphics 1996; 161035-1054. Link
11. Levine MS, Megibow AJ. Gastric Carcinoma. In: Gore RM, Levine MS, Laufer I, eds. Textbook of gastrointestinal radiology. Philadelphia: WB Saunders, 1994:600-683.
12. Rossi M, Broglia L, Maccioni F, et al. Hydr0-CT in patients with gastric cancer: preoperative radiologic staging. Eur Radiol 1997; 7:659-664. Medline
13. Hori S, Tsuda K, Murayama S, Matsushita M. CT of gastric carcinoma: preliminary results with a new scanning technique. RadioGraphics 1992; 12:257-268. Link
14. Baert AL, Roex L, Marchal G, Hermans P, Dewilde D, Wilms G. Computed tomography of the stomach with water as an oral contrast agent: technique and preliminary results. Jour Comput Assist Tomogr 1989; 13:633-636. Medline
15. Hundt W, Braunschweig R, Reiser M. Assessment of gastric cancer: value of breathhold technique and two phase spiral CT. Eur Radiol 1999; 9:68-72. Medline
16. Mani NB, Suri S, Gupta S, Wig JD. Two-phase dynamic contrast-enhanced computed tomography with water-filling method for staging gastric cancer. Clin Imaging 2001; 25:38-43. Medline
17. Lee DH, Ko YT. The role of 3D spiral CT in early gastric carcinoma. Jour Comput Assist Tomogr 1998; 22:709-713. Medline
18. Lee DH, Ko YT. Advanced gastric carcinoma: the role of three-dimensional and axial imaging by spiral CT. Abdom Imaging 1999; 24:111-116. Medline
19. Hopper KD, Iyriboz AT, Wise SW, Neuman JD, Mauger DT, Kasales CJ. Mucosal detail at CT virtual reality: surface vs. volume rendering. Radiology 2000; 214:517-522. Link
20. Wood BJ, O'Malley ME, Hahn PF, Mueller PR. Virtual endoscopy of the gastrointestinal system outside the colon. AJR 1998; 171:1367-1372. Medline
21. Megibow AJ, Balthazar EJ, Naidich DP, Bosniak MA. Computed tomography of gastrointestinal lymphoma. AJR 1983; 141:541-547. Medline
22. Buy JN, Moss A. Computed tomography of gastric lymphoma. AJR 1982; 138:859-865. Medline
23. Brown JA, Carson BW, Gascoyne RD, Cooperberg PL, Connors JM, Mason AC. Low grade gastric MALT lymphoma: radiographic findings. Clin Radiol 2000; 55:384-389. Medline
24. Kessar P, Norton A, Rohatiner AZ, Lister TA, Reznek RH. CT appearances of mucosa-associated lymphoid tissue (MALT) lymphoma. Eur Radiol 1999; 9:693-696. Medline
25. Peng SS, Tsang YM, Lin JT, Wang HH, Chiang IP, Hsu JC. Radiographic and computed tomographic findings of gastric mucosa-associated lymphoid tissue lymphomas. J Formos Med Assoc 1998; 97:261-365. Medline
26. Occhionorelli S, Mitaritonno M, Penella A, et al. Gastrointestinal stromal tumor (GIST): case report. G Chir 2001; 22:65-69. Medline
27. McLeod AJ, Zornoza J, Shirkoda A. Leiomyosarcoma: computed tomographic findings. Radiology 1984; 152:133-136. Link
28. Pannu HK, Hruban RH, Fishman EK. CT of gastric leiomyosarcoma: patterns of involvement. AJR 1999; 173:369-373. Medline
29. Gore RM, Levine MS, Laufer I. Textbook of gastrointestinal radiology. Philadelphia: Saunders, 1994:703-708.
30. Urban BA, Fishman EK, Hruban RH. Helicobacter pylori gastritis mimicking gastric carcinoma at CT evaluation. Radiology 1991; 179:689-691. Link
31. Jacobs JM, Hill MC, Steinberg WM. Peptic ulcer disease: CT evaluation. Radiology 1991; 178:745-748. Link
32. Shipman PJ, Drury P. Emphasematous gastritis: case report and literature review. Australas Radiol 2001; 45:64-66. Medline
33. Balthazar EJ, Megibow AJ, Naidich DP, LeFleur RS. Computed tomographic recognition of gastric varices. AJR 1984; 142:1121-1125. Medline
34. Matsumoto A, Kitamoto M, Imamura M, et al. Three-dimensional portography using multislice helical CT is clinically useful for management of gastric fundic varices. AJR 2001; 176:899-905. Medline
35. Ohasi I, Ina H, Hanafusa K, Yoshida T, et al. Aberrant left gastric vein, demonstrated by helical CT. J Comput Assist Tomogr 1997; 1997:6. Medline